Breast Cancer
Breast cancer is a serious health concern, and the most rampant form of cancer in Filipino women. According to doctors, they have estimated that breast cancer will develop in 3 out of 100 Filipino women during their lifetime.
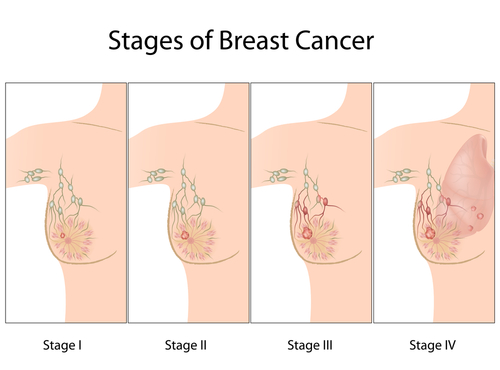
A lump in the breast or an abnormal mammogram are the first signs of breast cancer. Breast cancer can be diagnosed in stages ranging from early, curable, and advanced, wherein it has already spread.
- A lump in the breast or underarm that lingers even after your menstrual cycle is the first symptom of breast cancer. They are usually painless, but some may have a stinging sensation. A mammogram can detect lumps that aren’t seen or felt through a self breast examination.
- Swelling in the armpit.
- Pain or tenderness in the breast.
- Noticeable flattening or indentation on the breast, which may be a sign of an unseen or unfelt tumor.
- Change in size, shape, texture, or temperature of the breast. Advanced breast cancer may make your breast have a reddish color and a pitted surface, like the skin of an orange.
- Any change in the nipple, such as retraction, dimpling, itching, a burning sensation, or forming ulcers.
- Odd discharge from the nipple. It may be clear, bloody, or any other color. In some cases, this may be a sign of cancer.
- An area that feels like there’s a marble underneath the skin.
- An area that is noticeably different from other areas of the breasts.
Breast cancer screenings, such as breast exams or mammograms, help detect breast cancer in its earliest, most treatable stage.
Cervical Cancer
Cervical cancer mainly affects the cervix, the lower, narrow end of the uterus. In the Philippines, it is the 2nd leading form of cancer, with an estimation of 7,277 new cases and 3,807 deaths expected every year.
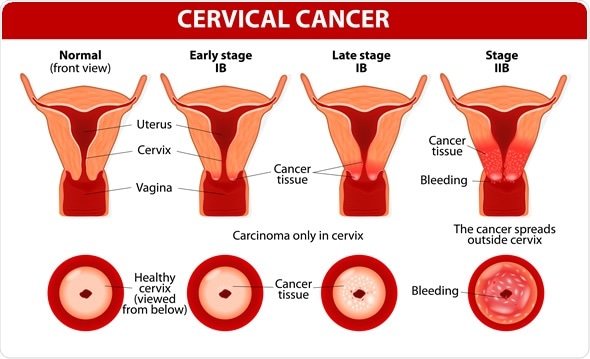
A high-risk type of HPV (human papillomavirus) is the leading cause of cervical cancer cases. The HPV virus is passed from one person to another through genital contact, such as vaginal, anal, or oral sex. It may cause cancer over time if the HPV infection does not clear on its own. There are also other factors that may further increase the risk of developing cancer after having a high-risk HPV infections. These factors are:
- Smoking
- Having HIV (human immunodeficiency virus), or reduced immunity
- Taking birth control pills for a long time (more than five years)
- Having given birth to three or more children
Getting the HPV vaccine can protect you from developing cervical cancer, and has already been available and used in the Philippines for decades. Ask your healthcare provider about the vaccine. Using condoms during sex can also prevent the spread of HPV and protect you from getting it. Cervical cancer can also be detected early through regular pelvic exams.
Ovarian Cancer
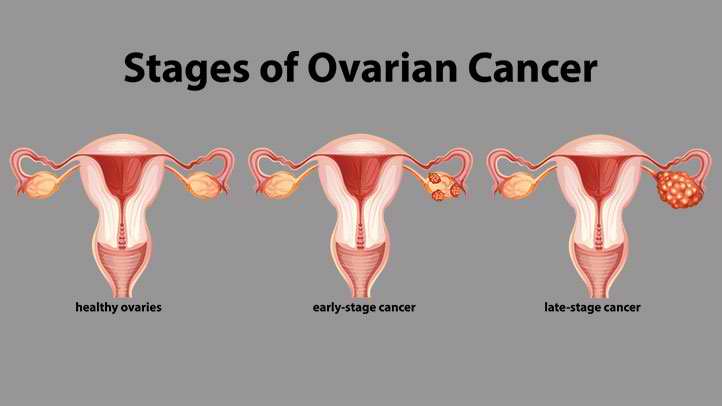
Ovarian cancer primarily starts in the ovaries, which are found on each side of the uterus. The ovaries are responsible for producing female hormones and egg cells. Ovarian cancer is a serious health concern, and more common in older women. Treatment is most effective when the cancer is detected early.
Symptoms
- Pain in the pelvis or abdomen (belly)
- Bloating in the abdomen
- Urinary urgency (needing to pee right away)
- Urinary frequency (having to pee often)
- Constipation or diarrhea
- Feeling full quickly while eating
- Having difficulty eating
- Vaginal bleeding or other discharge that is different than normal
- Back pain
Uterine Cancer
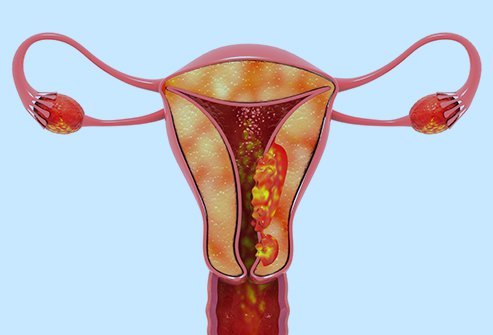
Uterine cancer affects the womb, the hollow, pear-shaped organ where a baby develops during pregnancy. There are different types of uterine cancers, and they include endometrial cancer and uterine sarcomas. The more common type between the two is endometrial cancer, and this happens when the cancer begins in the endometrium, the tissue lining of the uterus. When the cancer grows in the muscles or other supporting tissues in the uterus, this is a case of uterine sarcomas. It accounts for only a small portion of cancers of the uterus.
Vaginal Cancer
Vaginal cancer occurs when malignant (cancer) cells form in the vagina, the hollow tube-like canal connecting the cervix (the opening of the uterus) and the outside of the body. The vagina is also called the birth canal because when giving birth, this is where a baby passes through to exit the body.
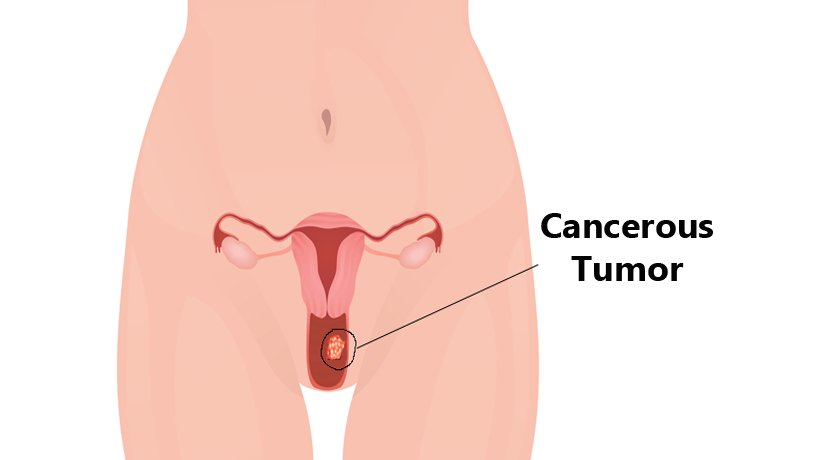
Vaginal cancer is not common. There are two main types of vaginal cancer:
Squamous cell carcinoma: The most common type of vaginal cancer. It forms in squamous cells, the thin, flat cells lining the vagina, and spreads slowly and usually stays near the vagina. It may also spread to the lungs, liver, or bone.
Adenocarcinoma: Cancer that begins in glandular (secretory) cells, which are cells found in the lining of the vagina. Glandular cells are responsible for making and releasing fluids such as mucus. Adenocarcinoma is more likely than squamous cell cancer to spread to the lungs and lymph nodes. A rare type of adenocarcinoma is linked to being exposed to diethylstilbestrol (DES) before birth, while adenocarcinomas that are not linked with being exposed to DES are most common in women after menopause.
“Risk factor” is the term used to refer to anything that contributes to the increased risk of getting a disease. Having a risk factor does not mean that you will surely develop cancer, and not having a risk factor does not guarantee that you will not get cancer. Consult your doctor if you think you may be at risk. The following are risk factors for vaginal cancer:
- Being aged 60 or older.
- Being exposed to DES while in the mother’s womb. In the 1950s, the drug DES was given to some pregnant women to prevent miscarriage (premature birth of a fetus that cannot survive). Women who were exposed to DES before birth have an increased risk of vaginal cancer. Some of these women develop a rare form of vaginal cancer called clear cell adenocarcinoma.
- Having HPV infection.
- Having a history of abnormal cells in the cervix, or cervical cancer.
- Having a history of abnormal cells in the uterus, or cancer of the uterus.
- Having had a hysterectomy due to health problems that affect the uterus.
Sources:
http://www.webmd.com/cancer/cervical-cancer/default.htm
https://www.doh.gov.ph/Health-Advisory/Uterine-Cervix-Cancer
https://www.pna.gov.ph/articles/1063773




Ask something really bothered to me.. I encountered some abnormal flow of my menstruation a month ago, I’m just spotting for the 3days covered of my period apparently, it should be consumed/used 1pack of sanitary napkins (8’s), I’m worried about this matter..
Hi Alyzza! Abnormalities in menstrual flow can be caused by a lot of factors, and sometimes stress, a sudden change in diet, and too much weight loss or weight gain can also be possible reasons for this. It’s best to see an OBGYN soon so they can check what’s causing the abnormalities you’re experiencing, and you’ll find out whether you need any medicine or changes in lifestyle. Watch out for any other symptoms, and the OBGYN everything you’re experiencing.