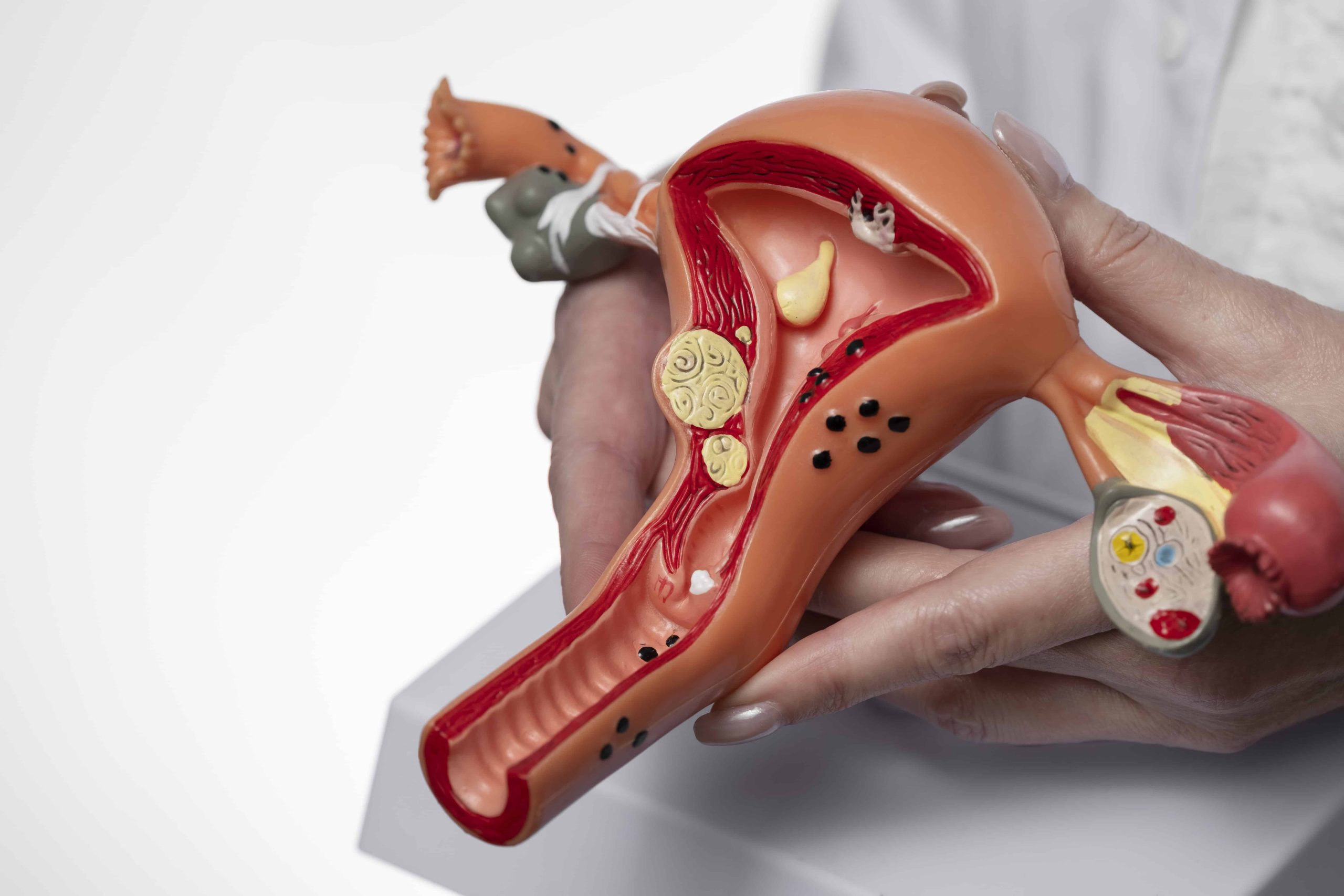
Do you experience…
- Intense period pains (dysmenorrhea) that can’t be relieved by rest, painkillers, or a hot compress?
- Heavy periods or bleeding in between periods?
- Pain or bleeding during sex, even if you’re not on your period?
- Irregular bowel movements or stomach problems?
- Lower back pains anytime in your menstrual cycle?
If you ticked off two or more of these symptoms, better have a chat with your OB/GYN about it. They can evaluate whether or not you have endometriosis.
Endometriosis is a condition in which the endometrium (the uterine lining) grows outside of the uterus, such as on the ovaries, fallopian tubes, bowel, and tissues lining the pelvis.
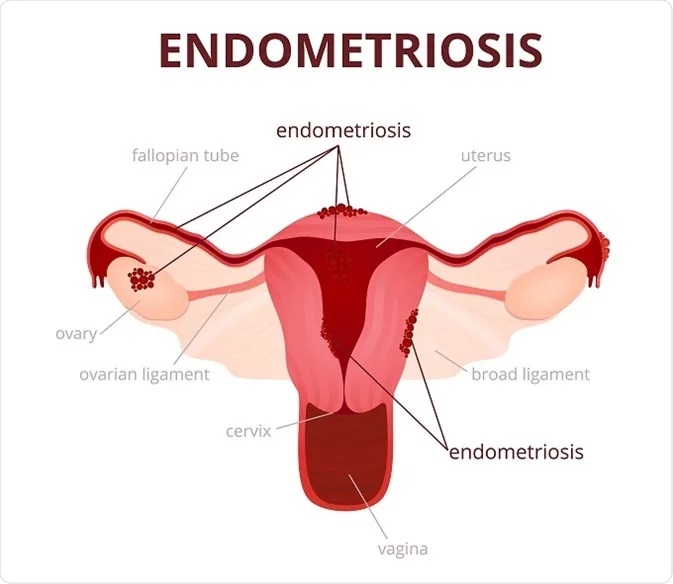
With endometriosis, the “lost” tissue would also act just like how the endometrium would. It thickens, sheds, and bleeds as well as you menstruate. But since it has no way to exit your body, it gets trapped inside and can cause:
- Irritation
- Scar formation
- Adhesions (wherein the tissue makes your pelvic organs and other tissues stick together)
- Severe pain during periods
- Fertility problems
Pelvic pain is the primary symptom of endometriosis, but the severity doesn’t indicate the degree or extent of the condition. Some may have a mild case but experience unbearable pain. Others could be in an advanced stage but feel little pain. You might even have no symptoms at all!
There are other conditions that also cause pelvic pains. Sometimes endometriosis can be mistaken for these instead, such as pelvic inflammatory disease (PID) or ovarian cysts. This is why it’s important to visit your gynecologist to get checked regularly. Getting proper and early diagnosis allows you to get the right treatment and to better manage the symptoms.
What are possible treatments for endometriosis?
The pain and other symptoms of endometriosis can really be bothersome, and hinder you from carrying out your daily activities. While there is no cure for endometriosis, there are treatment options to help ease and manage the symptoms.
There are medical and surgical options that can reduce symptoms and manage potential complications. Everyone may have different reactions to these treatments, but the right and best option for you depends on your doctor’s findings and diagnosis. These treatment options include:
Painkillers
Over-the-counter pain medications like ibuprofen may work for some women, but others may see that this isn’t enough to relieve the pain.
Hormonal therapy and contraceptives
Supplemental hormones may ease pain and stop the progression of endometriosis. Hormone therapy helps the body regulate changes in hormone levels that make the tissue grow.
Hormonal contraceptives such as oral contraceptive pills and injectables help prevent the monthly growth and buildup of the lost endometrial tissue, which relieves pain and other symptoms.
Surgery
Surgery is often recommended as a last resort if your condition doesn’t seem to be improving with the other treatments.
A conservative surgery may be recommended to women who plan to get pregnant or to women who experience severe pain that does not seem to be alleviated by hormonal treatments. In this type of surgery, the doctor removes or destroys endometrial growths.
A total hysterectomy might be recommended as a last resort for those whose condition does not seem to be responding to the other treatments. This surgery is done by removing the uterus, cervix, and ovaries, as well as visible implant lesions of the endometrial tissue. Pregnancy is impossible after a total hysterectomy, so think about it very carefully before deciding to undergo the surgery especially if you want to have your own family.
What are the possible complications of endometriosis?
The primary complication of endometriosis is infertility. Medications will only manage symptoms, but will not improve fertility. Even so, a lot of women with mild to moderate conditions are still able to conceive and have a normal pregnancy. Some are able to conceive after a conservative surgery, while others may need to consider fertility treatments or in vitro fertilization to increase chances of getting pregnant.
Even if fertility is not your concern, it’s always best to talk to your doctor about your condition and have yourself assessed.
Sources:
https://www.healthline.com/health/endometriosis
https://www.mayoclinic.org/diseases-conditions/endometriosis/symptoms-causes/syc-20354656